Our EHR Software unifies practice-wide functions, including patient management, scheduling, billing, and documentation, optimizing efficiency and coordination within healthcare facilities.
In the fast-paced healthcare industry, it is essential to prioritize efficiency and precision to deliver exceptional patient care. With our innovative approach to the design of EHR software solutions, healthcare providers can easily navigate the fast-paced healthcare industry and deliver exceptional patient care.
Our EMR software automates clinical and financial workflows of a practice and is fully customizable, significantly improving provider efficiency and clinical care. Transform your practice with our all-in-one integrated EHR that includes medical charting, practice management, e-prescribing, imaging, patient engagement, and medical billing to optimize overall healthcare management. Benefit from:
Experience the difference EMR from RevenueXL can make in your healthcare journey. Transform your practice with streamlined clinical workflows and join thousands of satisfied healthcare professionals who have benefited from our solutions.
Request a free demo today.


With our Electronic Health Records software, your practice can significantly enhance efficiency, accuracy, and quality of care.

Say goodbye to the complexities of traditional prescription methods with our EHR Software's robust e-Prescribing and medication management features. Providers can electronically generate and transmit prescriptions directly to pharmacies, streamlining the prescription fulfillment process and reducing the risk of medication errors.
Our EHR's medication management capabilities offer a comprehensive view of a patient's complete medication history, including current prescriptions, past medications, and allergies. This insight supports accurate medication reconciliation and promotes patient adherence to prescribed regimens. By leveraging our EMR's e-Prescribing and medication management functionalities, your practice can enhance patient safety, improve prescription accuracy, and optimize medication-related workflows.

Financial efficiency is a critical aspect of a successful healthcare practice and they must be able to streamline billing and revenue cycle management, ensuring that their practice remains financially healthy while focusing on delivering exceptional patient care.
Automated charge capture functionalities reduce the risk of missed charges and claim denials, maximizing revenue potential. The EMR's coding assistance tools help ensure accurate and compliant coding, reducing the likelihood of billing errors. Furthermore, built-in claim scrubbing and validation features help identify potential issues before claims are submitted, reducing claim rejection rates and accelerating reimbursement cycles.
With comprehensive reporting capabilities, your practice can gain valuable insights into revenue streams, claim performance, and financial trends. Our EMR's billing and revenue cycle management features empower your practice to optimize financial processes, improve revenue capture, and enhance overall financial performance.

In today's data-driven healthcare landscape, extracting meaningful insights from patient information is crucial. Such meaningful insights empower healthcare providers to make data-informed decisions and drive continuous quality improvement.
Providers can monitor key performance indicators (KPIs), track patient outcomes, and identify trends through customizable dashboards and in-depth reports. Access to clinical and financial data enables proactive intervention and the implementation of evidence-based best practices to enhance patient care.
By leveraging our EMR's analytical capabilities, your practice can identify areas for improvement, optimize workflows, and enhance overall operational efficiency. Furthermore, these insights facilitate compliance with quality reporting initiatives and regulatory requirements, positioning your practice for success in value-based care models.
Incorporating telemedicine into your practice is now easier than ever with our EMR software's telemedicine capabilities. Offer patients the convenience of virtual visits while maintaining the same level of care as in-person appointments.
Through secure and HIPAA-compliant video conferencing, providers can connect with patients in real-time, irrespective of geographic barriers. Telemedicine expands access to care, especially for patients in remote areas or with limited mobility, leading to improved patient engagement and satisfaction.
With our telemedicine platform that seamlessly integrates with existing EHR workflows, providers can document virtual visits directly in patient records. Embrace the future of healthcare with telemedicine, and provide your patients with flexible care options that prioritize convenience, accessibility, and quality.
Customized templates and workflow for your specialty to accelerate adoption, encounter documentation speed and patient care.
Ready to see how RevenueXL can help your medical practice improve efficiency and enhance quality of patient care?
Fill out the form below to request your customized EMR Software demo.
Implementing integrated EMR (Electronic Medical Records) and Practice Management Software is a strategic decision that can revolutionize how healthcare practices operate and deliver patient care. By combining these two essential systems into one cohesive solution, healthcare providers can experience numerous benefits that enhance efficiency, productivity, and patient outcomes. Here's why you should consider adopting integrated EMR and Practice Management Software:
1. Streamlined Workflows: Integrated software allows seamless data sharing between EMR and Practice Management, eliminating duplicate data entry and reducing administrative burdens. This results in streamlined workflows and more time for patient care.
2. Improved Patient Engagement: Access to integrated patient information enables more personalized care and better patient engagement. Providers can access medical histories, treatment plans, and billing details in one place, leading to more informed interactions with patients.
3. Enhanced Revenue Cycle Management: Integrated systems facilitate smooth billing and coding processes, reducing claim errors and accelerating reimbursement cycles. It ensures a more efficient revenue cycle management, positively impacting the practice's financial health.
4. Comprehensive Reporting and Analytics: Combined EMR and Practice Management Software offer comprehensive reporting and analytics capabilities. Providers can access real-time insights into practice performance, patient outcomes, and financial metrics, allowing for data-driven decision-making.
5. Better Care Coordination: Integrated systems enable seamless communication and care coordination among different departments within the practice. This fosters better collaboration, leading to improved patient care and outcomes.
6. Increased Data Security and Compliance: An integrated solution centralizes patient data, making it easier to implement robust security measures and ensure compliance with healthcare regulations.
7. Simplified Training and Support: Training staff on a single integrated system is more efficient than managing multiple software applications. Moreover, ongoing support and maintenance are streamlined with a unified solution.
By implementing integrated EMR and Practice Management Software, healthcare practices can optimize operations, elevate patient care, and position themselves for success in an increasingly digital healthcare landscape. It's a strategic investment that delivers long-term benefits and drives growth for the practice.
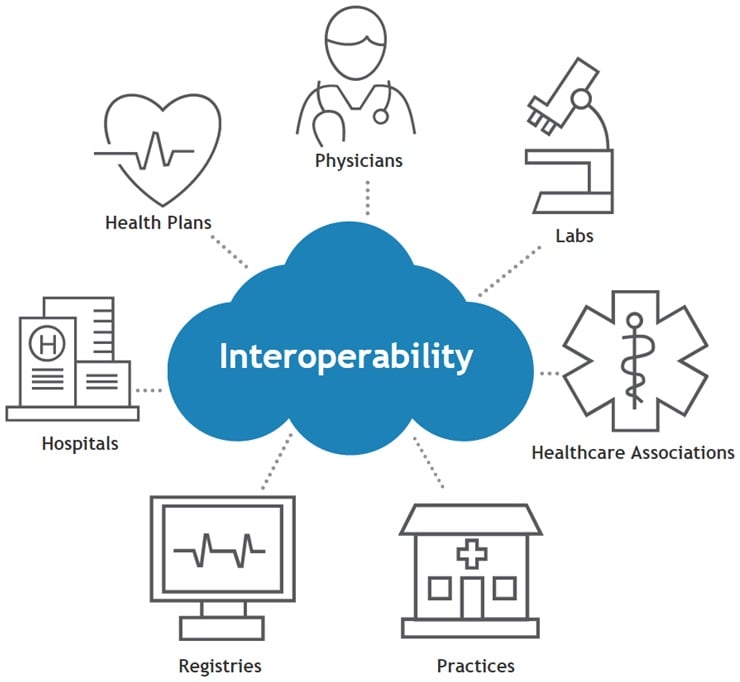
This question focuses on the interoperability of offered by our software. The ability to exchange and make use of information from other healthcare providers, such as laboratories and specialists, is a crucial feature of our EMR Software.
Healthcare providers have to comply with a number of regulations, such as HIPAA, which governs the handling of medical records. PrognoCIS supports compliance by ensuring proper security, consent management, and audit capabilities.
We have published a large number of educational resources and blog posts on our website.
Some resources listed below:
Differences between EMR and EHR
“PrognoCIS is the perfect…system for us. This is our 3rd EMR system and by far better then [sic] then the others. We don’t have to worry about waiting til the next day to access a patient chart. Also very easy to use with [our] dictation system.”
– J. with P.B., MD
“We have been with PrognoCIS for 5 years after experiencing an epic failure with another EHR solution. Our practice is a small private medical office and flexibility is paramount to optimizing our functionality. What we like most about PrognoCIS is the adaptability or customization of the product.”
– A. from S.W. Clinic
“Streamlined, easy to use, and comprehensive! I can customize myself on the fly and I like the ability to…access on my PC, Apple (Mac or iPad at home) or via the iPhone app. After using a few other systems, I saw the designers of PrognoCIS truly understand how a clinical office functions.”
– S. Wellness Group
Streamline & automate administrative and clinical tasks, allowing providers to focus on patient care in safe manner
Two service options to ensure your MU attestations are smooth and hassle-free
Easily share lab results, appointment reminders, statements, and prescriptions with patients
Patients can complete secure credit card transactions from the comfort of their homes
RCM services process statements and handle claims while you connect with patients
Designed for specialty, from Allergy to Urology
Quickly prescribe or refill prescriptions and send straight to the patient’s preferred pharmacy
Surescripts feature allows you to monitor patient prescription usage and medication adherence
Friendly, knowledgeable 24/7 support staff available via support ticket, phone, email, or chat
Quickly enroll your practice with 3rd-party payers and begin seeing patients
Electronically sign documents within EMR or patient portal with HIPAA-compliant e-signature feature
HL-7 interfacing and CCHIT & ONC-ATCB-certified, conforming to critical security and functionality measures
Communicate with practice & labs, radiology, pharmacies, & referring doctors
Convenient with iPhone & iPad
© 2021 RevenueXL Inc. All rights reserved. Unauthorized Reproduction Prohibited - Legal Notice.