Elevate your practice with convenient appointment scheduling, efficient billing and invoicing, patient management, insightful analytics, and seamless integration with other healthcare systems
In today's dynamic landscape of medical practice management, maximizing efficiency and accuracy is paramount for delivering top-tier patient care. Our cloud-based electronic health record is integrated with the practice management software you need to navigate the complexities of practice management with ease, ensuring seamless operations and top-notch patient care.
Practice management software streamlines and optimizes healthcare operations with tools for appointment scheduling, reminders, eligibility verification, and medical billing, empowering staff to focus on patient care.
Transform your practice with our integrated EMR and Practice Management Software today and feel the transformative power of unified systems and intuitive features in your healthcare journey. Request a free demo today.
Solutions to Maximize Your Practice Efficiency







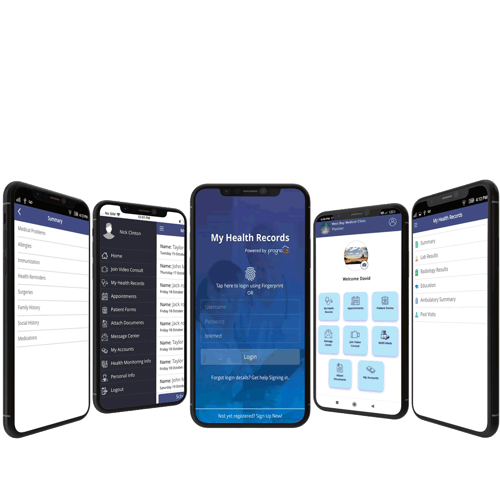
Universal Secure Access: Connect seamlessly via any internet-enabled device—tablets, smartphones, PCs, or Macs—with two-factor authentication ensuring data security. Send appointment reminders, view lab results, and streamline communication.
Integrated Patient Tools: Check and request appointments, view statements, and ask for prescription refills. Facilitate rapid communication with other healthcare providers, ensuring cohesive patient care without delays.
Boosted Engagement & Efficiency: Enhance patient engagement, loyalty, and health outcomes. Simplify administrative tasks with online forms and patient-driven scheduling, all within a HIPAA-compliant environment.

Streamlined Team Communication: Advanced internal messaging systems ensure seamless synchronization among staff members. With these tools, communication gaps are eliminated, fostering unified care and bolstering administrative efficiency.
Direct & Secure Patient Interactions: Prioritizing the bond between patients and healthcare providers, integrated tools facilitate appointment reminders, health updates, and real-time feedback. This fosters trust, ensuring patients remain informed and engaged every step of their health journey.
Integrated Alerts & Automated Notifications: Tailored notifications and alerts enhance patient adherence, ensuring they’re kept abreast of upcoming appointments, medication schedules, and essential health milestones.
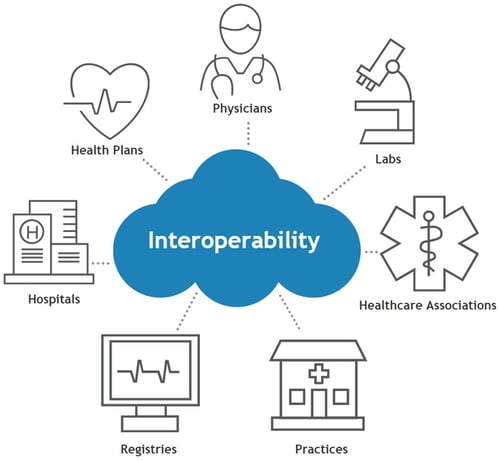
Advanced System Synchronization: RevenueXL stands out in its ability to harmoniously interact with a multitude of platforms, breaking data silos and ensuring a comprehensive patient care approach by maintaining up-to-date information across various systems.
Open System Adaptability: Embracing an Open API infrastructure, RevenueXL offers unparalleled flexibility, allowing for easy integration with a wide range of third-party apps and tools, positioning practices to remain adaptable to the ever-evolving healthcare tech landscape.
Unified Healthcare Data Framework: Our commitment to real-time data synchronization ensures every stakeholder has access to the most current and comprehensive patient data, fostering effective clinical decisions and enhanced patient outcomes.
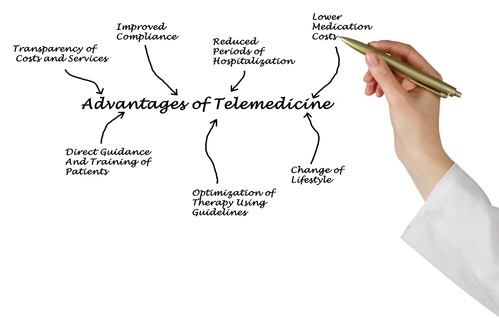
Holistic Patient Care: Bridging geographical barriers, the software offers patients, especially in underserved regions, swift access to expert diagnoses, treatments, and real-time care.
Optimized Virtual Engagement: Our custom mobile app blends text, email, and video, simplifying remote consultations and bolstering patient-provider interactions while lowering costs.
Unparalleled Access & Integration: Within a HIPAA-compliant framework, physicians can access patient charts, prescribe medications, and seamlessly liaise with other healthcare departments.
Scalability and Connectivity: Perfect for solo practitioners to large medical facilities, RevenueXL ensures smooth communication with essential healthcare entities, centralizing critical interactions.
Customized templates and workflow for your specialty to accelerate adoption, encounter documentation speed and patient care.
Ready to see how RevenueXL can help your medical practice improve efficiency and enhance quality of patient care?
Fill out the form below to schedule your customized EMR Software demo.
“PrognoCIS is the perfect…system for us. This is our 3rd EMR system and by far better then [sic] then the others. We don’t have to worry about waiting til the next day to access a patient chart. Also very easy to use with [our] dictation system.”
– J. with P.B., MD
“We have been with PrognoCIS for 5 years after experiencing an epic failure with another EHR solution. Our practice is a small private medical office and flexibility is paramount to optimizing our functionality. What we like most about PrognoCIS is the adaptability or customization of the product.”
– A. from S.W. Clinic
“Streamlined, easy to use, and comprehensive! I can customize myself on the fly and I like the ability to…access on my PC, Apple (Mac or iPad at home) or via the iPhone app. After using a few other systems, I saw the designers of PrognoCIS truly understand how a clinical office functions.”
– S. Wellness Group
Customizable workflow,templates, and content created for your specialty
Two service options to ensure your MU attestations are smooth and hassle-free
Easily share lab results, appointment reminders, statements, and prescriptions with patients
Patients can complete secure credit card transactions from the comfort of their homes
RCM services process statements and handle claims while you connect with patients
Designed for specialty, from Allergy to Urology
Quickly prescribe or refill prescriptions and send straight to the patient’s preferred pharmacy
Surescripts feature allows you to monitor patient prescription usage and medication adherence
Friendly, knowledgeable 24/7 support staff available via support ticket, phone, email, or chat
Quickly enroll your practice with 3rd-party payers and begin seeing patients
Electronically sign documents within EMR or patient portal with HIPAA-compliant e-signature feature
HL-7 interfacing and CCHIT & ONC-ATCB-certified, conforming to critical security and functionality measures
Communicate with practice & labs, radiology, pharmacies, & referring doctors
Convenient with iPhone & iPad
© 2021 RevenueXL Inc. All rights reserved. Unauthorized Reproduction Prohibited - Legal Notice.