Discover an EHR designed to enhance patient care and streamline clinical workflows. Simplify your practice operations and increase efficiency through customizable specialty-specific templates and integrated tools for scheduling, e-prescribing (eRx), telehealth, lab integration, billing, and revenue cycle management.
Whether you're running a solo practice or a small clinic, our solutions reduce charting time, minimize errors, and streamline your clinical and administrative operations—helping you focus more on patients and less on paperwork.
Discover how the right EMR can reduce charting time, improve care continuity, and simplify daily operations—so your team can focus more on patients and less on paperwork.





Simplify prescription management with advanced e-Prescribing and medication management features.
Access a detailed view of each patient’s medication history:
Leverage these capabilities to:

Financial efficiency is essential for a thriving healthcare practice, enabling streamlined billing and revenue cycle management to maintain financial health while prioritizing exceptional patient care.
Key features that support financial efficiency include:
Comprehensive reporting capabilities provide:
By leveraging advanced billing and revenue cycle management features, your practice can:

In today’s data-driven healthcare environment, uncovering actionable insights from patient information is vital for informed decision-making and continuous quality improvement.
Providers can leverage advanced analytics to:
Access to clinical and financial data enables:
By utilizing our analytical tools, your practice can:
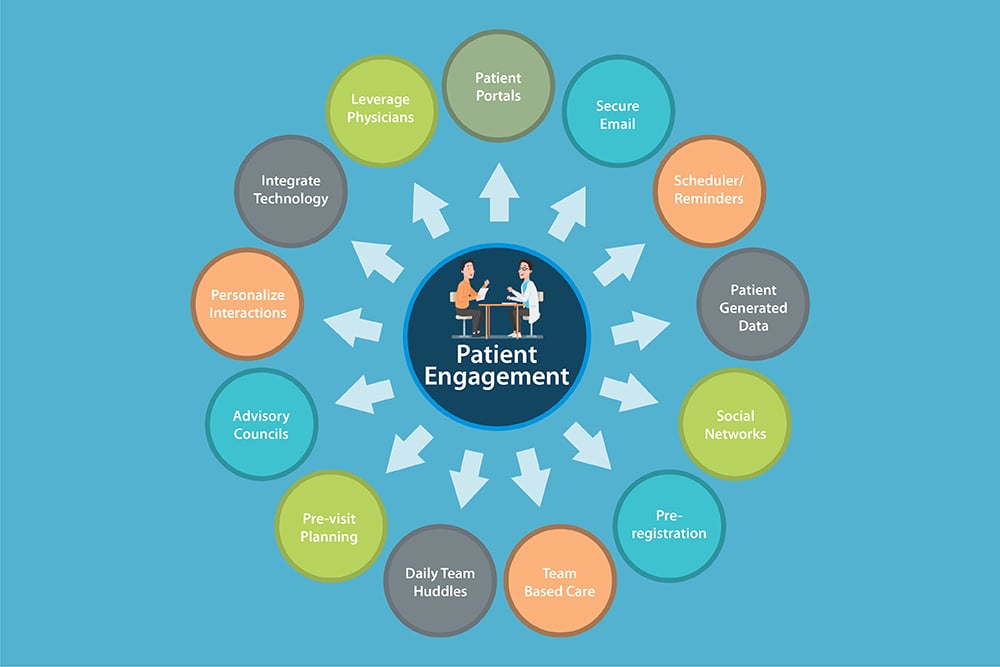
Patient Engagement Tools and Secure Patient Portal:
By fostering patient engagement, RevenueXL:
Customized templates and workflow for your specialty to accelerate adoption, encounter documentation speed and patient care.
Ready to see how RevenueXL can help your medical practice improve efficiency and enhance quality of patient care?
Fill out the form below to request your customized demo.
Implementing integrated EMR (Electronic Medical Records) and Practice Management Software is a strategic decision that can revolutionize how healthcare practices operate and deliver patient care. By combining these two essential systems into one cohesive solution, healthcare providers can experience numerous benefits that enhance efficiency, productivity, and patient outcomes. Here's why you should consider adopting integrated Software:
1. Streamlined Workflows: Integrated software allows seamless data sharing between EMR and Practice Management Software, eliminating duplicate data entry and reducing administrative burdens. This results in streamlined workflows and more time for patient care.
2. Improved Patient Engagement: Access to integrated patient information enables more personalized care and better patient engagement. Providers can access medical histories, treatment plans, and billing details in one place, leading to more informed interactions with patients.
3. Enhanced Revenue Cycle Management: Integrated systems facilitate smooth billing and coding processes, reducing claim errors and accelerating reimbursement cycles. It ensures a more efficient revenue cycle management, positively impacting the practice's financial health.
4. Comprehensive Reporting and Analytics: Integrated software enables comprehensive reporting and analytics capabilities. Providers can access real-time insights into practice performance, patient outcomes, and financial metrics, allowing for data-driven decision-making.
5. Better Care Coordination: Integrated software enable seamless communication and care coordination among different departments within the practice. This fosters better collaboration, leading to improved patient care and outcomes.
6. Increased Data Security and Compliance: An integrated solution centralizes patient data, making it easier to implement robust security measures and ensure compliance with healthcare regulations.
7. Simplified Training and Support: Training staff on a single integrated system is more efficient than managing multiple software applications. Moreover, ongoing support and maintenance are streamlined with a unified solution.
By implementing integrated EMR and Practice Management Software, healthcare practices can optimize operations, elevate patient care, and position themselves for success in an increasingly digital healthcare landscape. It's a strategic investment that delivers long-term benefits and drives growth for the practice.
This question focuses on the interoperability of offered by our software. The ability to exchange and make use of information from other healthcare providers, such as laboratories and specialists, is a crucial feature of our EMR.
Healthcare providers have to comply with a number of regulations, such as HIPAA, which governs the handling of medical records. PrognoCIS supports compliance by ensuring proper security, consent management, and audit capabilities.
We have published a large number of educational resources and blog posts on our website.
Some resources listed below:
Full compliance with HIPAA regulations is ensured while safeguarding patient data through the following key measures:
With these protections, our Electronic Medical Records Software ensures the confidentiality, integrity, and security of patient data, giving healthcare providers peace of mind.
Providers can customize their clinical workflows and individual templates
Two service options to ensure your MU attestations are smooth and hassle-free
Easily share lab results, appointment reminders, statements, and prescriptions with patients
Patients can complete secure credit card transactions from the comfort of their homes
RCM services process statements and handle claims while you connect with patients
Designed for specialty, from Allergy to Urology
Quickly prescribe or refill prescriptions and send straight to the patient’s preferred pharmacy
Surescripts feature allows you to monitor patient prescription usage and medication adherence
Friendly, knowledgeable 24/7 support staff available via support ticket, phone, email, or chat
Quickly enroll your practice with 3rd-party payers and begin seeing patients
Electronically sign documents within EMR or patient portal with HIPAA-compliant e-signature feature
HL-7 interfacing and CCHIT & ONC-ATCB-certified, conforming to critical security and functionality measures
Communicate with practice & labs, radiology, pharmacies, & referring doctors
Convenient with iPhone & iPad
© 2021 RevenueXL Inc. All rights reserved. Unauthorized Reproduction Prohibited - Legal Notice.