Contrary to what you may believe, medical billing is more than just creating claims based on CPT and ICD codes provided by the coders and submitting them.
Medical billing is the process of reviewing patient records, applying standardized codes, and submitting claims to insurance companies to obtain payment for medical services. It also includes verifying coverage and following up on claims to ensure providers get paid for the care delivered, supporting timely reimbursements and stable revenue cycles.
This process demands constant attention and diligent follow-up to ensure healthcare providers receive the compensation they deserve for their valuable work. Therefore, healthcare providers must work with experienced medical billing professionals who can handle this process effectively. With their expertise and attention to detail, these professionals can ensure that healthcare providers receive prompt and accurate payment for the services rendered. So, if you're a healthcare provider looking to streamline your billing process and maximize your revenue, it's time to partner with a team of skilled medical billing professionals who can help you achieve your goals.
Many claims denied due to missing or incorrect data, duplicate or late submissions, improper or outdated CPT or ICD-10 codes, lack of documentation or prior authorization, and other reasons can be corrected and appealed. The goal is to ensure that the healthcare provider is reimbursed for the services they have provided to a patient.
The emergence of multiple technologies in the healthcare industry has transitioned medical billing processes from paper-based and handwritten or typewriter-drafted documents to electronic ones. This has saved time and money and reduced human and administrative errors.
Types
There are several types of medical billing, including:
-
Professional Medical Billing: This type of billing is used by individual healthcare providers, such as physicians, dentists, and chiropractors, to bill for services they provide to patients.
-
Institutional Medical Billing: Hospitals, clinics, and other healthcare facilities use this type of billing to bill for services provided to patients.
-
Medicare Billing: This type of billing is used specifically for billing services to Medicare, a federal health insurance program for people over 65 years of age or with certain disabilities.
-
Medicaid Billing: This type of billing is used specifically for billing services to Medicaid, a joint federal and state health insurance program for people with low income and limited resources.
-
Workers' Compensation Billing: This type of billing is used to bill for healthcare services provided to employees injured on the job and covered by workers' compensation insurance.
-
Personal Injury Billing: This type of billing is used to bill for healthcare services provided to patients injured due to an accident or other personal injury, and the responsible party's liability insurance covers their medical bills.
Each type of medical billing has its own specific requirements and regulations, and the billing process can vary depending on the type of billing being used. Healthcare providers and medical billing specialists need to understand the different types of medical billing to effectively navigate the billing process and ensure accurate and timely payment for healthcare services.
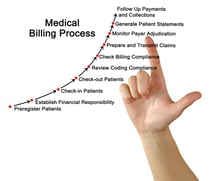
Learn more about the 11 steps of the billing lifecycle
There are several business processes that play an important part in ensuring that a physician's practice receives the revenue it is owed. If any of these steps are missed or done incorrectly, it can negatively affect the practice’s revenue cycle.
1. Patient registration
- This step collects and verifies patient demographic information, insurance information, and medical history.
- Includes basic information such as name, address, date of birth, insurance information, and any medical conditions or allergies.
Accurate and up-to-date patient registration is essential for ensuring that medical billing is accurate and efficient.
2. Charge capture
- Involves accurately documenting patient services, including diagnostic and treatment codes.
- Includes documenting the types and quantity of services and associated charges.
Charge capture is essential for ensuring insurance companies can accurately reimburse healthcare providers for their services.
3. Coding of Diagnosis, Procedures and Modifiers
After patient check-out, the next step is translating the report from the visit into diagnosis and procedure codes. This includes charge validation and creation of a superbill, an itemized form that details services provided to a patient. It is thereafter submitted to a payer for reimbursement.
4. Claim submission
The claim includes supporting documentation such as codes and charge information. It is then submitted to insurance companies for reimbursement. Claim submissions must be accurate and complete to ensure timely reimbursement.
5. Insurance verification
- It means verifying a patient's insurance coverage and benefits.
- Includes checking for coverage, co-pays, deductibles, and out-of-pocket maximums.
Insurance verification is essential to ensure patients understand their financial responsibility and reduce the risk of uncompensated care.
6. Authorization and pre-certification
Authorization and pre-certification means obtaining prior approval from insurance companies for certain procedures or treatments.
- Includes obtaining authorization for a specific service or procedure, which may be required for surgeries or imaging tests.
Authorization and pre-certification are important for reducing the risk of denied claims.
7. Payment posting
Payment posting means a process of recording payments from insurance companies and patients.
- Includes recording the amount paid, the date of payment, and the payment source.
Payment posting is essential for ensuring healthcare providers accurately record their financial performance.
8. Denial management
When a claim is denied, the underlying reason must be identified and addressed, including appeals and re-submissions. This includes identifying the reason for the denial, preparing and submitting an appeal, and following up with the insurance company. Denial management is essential for reducing the risk of lost revenue and ensuring that healthcare providers receive full reimbursement.
9. Accounts receivable follow-up
Following up on outstanding accounts, including collections and bad debt management. This includes following up with patients and insurance companies to ensure payment is received promptly and may include sending reminders, making phone calls, and negotiating payment plans. Accounts receivable follow-up is essential for reducing the risk of lost revenue and improving financial performance.
10. Billing Report generation
This includes generating reports on revenue, expenses, collections, and denial rates, as well as generating reports for management and stakeholders. Report generation is essential for ensuring healthcare providers have the information they need to make informed decisions.
11. Compliance
Every practice must ensure that medical billing practices are in compliance with applicable regulations, including HIPAA, CMS, and state and federal laws. This includes ensuring that patient information is protected, that claims are submitted in accordance with regulations, and that billing practices are consistent with industry standards. Compliance is essential for reducing the risk of fines and penalties and ensuring that healthcare providers operate ethically and in the best interests of their patients.
Challenges
Healthcare providers that fail to streamline their medical billing process jeopardize the financial sustainability of their practice. However, by focusing on combating common challenges in the process, they can increase their reimbursement and optimize their revenue cycle. Key obstacles in medical billing include:
1. Denials
Claim denial occurs when a claim is processed and repudiated by a payer. Denials fall under five primary categories: soft, hard, preventable, clinical, and administrative. Most denied claims are preventable; over half can be re-submitted once corrected.
2. Accuracy
Some healthcare providers continue to manually perform their denial management process, often resulting in increased human errors and reduced transparency. Even the smallest amount of inaccurate or incomplete patient information can result in a claim being denied.
3. Patient Eligibility
The number one source for denied claims is patient eligibility, meaning the service submitted for payment isn’t included in the insurance plan under which it’s being billed. Front-office staff must ensure they verify a patient’s health insurance status and coverage.
4. Lack of Automation
Manual claim processes are usually extremely time-consuming and increase the turnaround for claims. Healthcare providers that lack automation in their medical billing process miss out on the capability for advanced claims reporting and customized decision support.
5. Lack of Technology
Without technology to effectively prioritize, manage, and channel claims, physician practices are unlikely to be able to streamline their denial management and obtain revenue they’re owed by patients and payers. Even if a practice’s staff members are knowledgeable about the process, not having the applicable technology to administer claims makes it difficult to manage them efficiently
Physician practices have had to deal with additional challenges the past few months due to the COVID-19 pandemic. Even with the Coronavirus Aid, Relief, and Economic Security (CARES) Act and updated billing guidance from the Centers for Medicare & Medicaid Services (CMS) healthcare professional services declined 68% in utilization and 48% in revenue compared to the same time period last year.
Patient visits are still approximately one-third lower than they were before the new coronavirus hit the United States, and many practices are trying different options to accrue extra revenue, including implementing telemedicine initiatives and adding other service lines to their offerings. Through streamlined medical billing, these healthcare providers can ensure their revenue cycle runs smoothly during both decreases in patient visits and backlogs of appointments.
Evolution of Medical Billing
Medical billing has evolved significantly over the last few years, driven by changes in the healthcare industry and advancements in technology. Some of the key changes include:
1. Increased use of electronic billing
Electronic billing has become more widespread, allowing for faster and more accurate claims processing. According to a study by the Healthcare Financial Management Association (HFMA), electronic billing reduces the time it takes to process a claim from 14 days to just two days.
2. Adoption of value-based care
With the shift toward value based care, medical billing has become more focused on outcome-based metrics, such as patient satisfaction and health outcomes. This has led to a greater emphasis on population health management and patient engagement.
3. Increased complexity of codes and regulations
With the adoption of new codes and regulations, medical billing has become more complex, requiring specialized expertise to navigate. A study by the Medical Group Management Association (MGMA) found that 92% of medical billing professionals find the current coding and reimbursement environment to be challenging.
4. Growth of patient financial responsibility
Patients are now responsible for an increasing portion of their healthcare costs, requiring medical billing teams to be more focused on patient collections and insurance verification. A survey by the Kaiser Family Foundation found that patient cost-sharing has increased by an average of 63% over the past decade.
5. Growing importance of patient collections
The shift from fee-for-service to value-based care has resulted in higher health insurance deductibles for some patients. In fact, patient costs, including out-of-pocket maximums and deductibles, have increased 30% over the past four years and 230% in the previous 10 years. Therefore, providers have had to adjust their collection strategies, including collecting payment before procedures, revising payment agreements, and promoting price transparency. Following are a few statistics that show why patient collections can be challenging for physician practices:
-
-
- It costs healthcare providers four times more to pursue debt collections with patients than to receive reimbursement from a payer.
- Patient copays make up about 20% of a doctor’s office revenue, but most physician practices only collect 60% of patient copays.
- Approximately 81% of self-pay net revenues go unrecovered and default at a rate of 30% or more, meaning it can cost twice as much to collect from a patient as it does from a payer.
- About 10% of a physician practice’s patient A/R in the 60-90-day bucket is the cost associated with that A/R, and practices with patients at 60-90 days outstanding (DSO) lose an average of $5,000 per month.
-
5. Emphasis on data analytics:
Data analytics is playing a growing role in medical billing, allowing healthcare providers to gain insights into their billing and collections processes, and identify opportunities for improvement. A study by Health Affairs found that data analytics can help healthcare organizations improve revenue cycle management and reduce administrative costs by up to 15%.
Sources:
-
- Healthcare Financial Management Association (HFMA), "Electronic Billing and Payment: Streamlining Claims Processing and Payment" (2017)
- Medical Group Management Association (MGMA), "Coding and Reimbursement" (2019)
- Kaiser Family Foundation, "Trends in Employer Health Coverage" (2022)
- Health Affairs, "Data Analytics in Healthcare: Opportunities and Challenges" (2021)
The Future of Medical Billing
Technology is expected to have a significant impact on the medical billing landscape, driving increased efficiency, accuracy, and security in the billing process, while also freeing up medical billing teams to focus on more strategic and patient-facing activities.
1. Artificial Intelligence (AI) and Machine Learning (ML)
AI and ML are expected to play an increasingly important role in medical billing, allowing for more efficient and accurate claims processing, as well as improved decision-making and revenue cycle management. AI algorithms can be used to identify and address billing errors and inefficiencies, while ML can be used to predict and prevent future issues.
2. Computer-assisted coding (CAC)
CAC has been shown to lower coding time by 22% without reducing accuracy and will probably continue to be used by physician practices in an attempt to increase productivity and reduce claim backlogs. For practices, it can prompt identification of gaps in clinical documentation and faster medical billing.
3. Blockchain
Blockchain technology is expected to play a role in improving the transparency and security of medical billing processes. Blockchain-based solutions can be used to ensure the accuracy of medical claims and secure the exchange of sensitive information between healthcare providers, payers, and patients.
4. Cloud Computing
Cloud computing is expected to continue to play a significant role in the medical billing landscape, allowing for more flexible and scalable billing solutions. By storing and processing data in the cloud, medical billing teams can access and analyze data in real-time, even when working remotely.
5. Robotic Process Automation (RPA)
RPA is expected to automate many of the manual and repetitive tasks involved in medical billing, such as claims submissions, insurance verifications, and collections. RPA can be used to improve the accuracy and speed of these tasks, while freeing up medical billing teams to focus on more strategic and patient-facing activities.
6. Telemedicine and Virtual Care
Telemedicine and virtual care are expected to play an increasingly important role in the delivery of healthcare services, and will require new medical billing solutions to ensure accurate billing for these services. This will include the development of new codes and reimbursement models for virtual services, as well as the integration of telemedicine platforms with medical billing systems.
Find out what makes RevenueXL’s medical billing services unique – contact us to schedule a demo.








